Abstract
Smart contacts are one of the newest platforms for smart technology. They couple a compact wearable device with equipment for health diagnostics and drug delivery, optimizing both the existing infrastructures of ophthalmology and general medicine. Smart contacts already have a wide potential customer base in patients who want improved quality of life and real-time health care, leading to increased research on the safety and efficacy of smart contacts. Similarly to how the cell phone industry absorbed features of landlines to broaden the target market, however, smart contacts will not stay forever in the medical diagnostic arena. Beyond treatment of pre-existing medical conditions, they may be used in the future in preventative healthcare initiatives and even extend into recreational use.
Introduction
We live in the age of the Avengers. Superheroes are not just brave men and women with large hearts and a strong moral compass, but include those ingenious enough to create their own superpowers. Tony Stark was not born with super strength or the power to fly, and Scott Lang could not naturally shrink to the size of an insect. Instead, they used intellect and science to turn themselves into the characters we have all grown to love. If there is any group in daily life that seeks to emulate these heroes, it is engineers. Engineers love to recreate gadgets from action and science fiction tales, and invent new devices not yet imagined. One of these emerging new devices, aligning with the Avengers humanitarian aim of helping people, is smart contacts.
Like regular contact lenses, smart contacts are flexible, biocompatible lenses that fit into the eye; however, they are fitted with extra features beyond corrective vision. These features usually include a microchip or integrated circuit, a radiofrequency (RF) antenna, and sometimes some form of indicator such as a color-changing compound or a light-emitting diode (LED) [1]. The immediate goal for smart contacts is use in disease monitoring and treatment, but the biomedical community also hopes to expand their applications into the common medical device sphere.
Necessary Considerations
The first barrier to smart contact development and implementation is the extensive list of requirements for an ocular medical device. The contacts need to be oxygen-permeable to allow the eye to breathe. If the contact lens obstructs the eye from oxygen, corneal neurovascularization, or the growth of excess blood vessels in the cornea, may occur. Corneal neurovascularization can lead to light sensitivity, pain, vision blurring, and intolerance to contact lenses. Furthermore, the contacts need to be affordable (especially considering the miniscule circuity with which they are equipped), non-toxic (since they are in the eye many hours per day), comfortable for the patient, and transparent. Finally, the circuitry within the contact lens must not only be safe and reliable within the aqueous environment of the eye, but also must be small enough so as not to obstruct the wearer’s vision.
Components
Manufacturers of smart contacts have already tackled the labyrinth of design considerations presented to them. For a transparent body of the contact lens, different companies have used two main materials: polydimethylsiloxane (PDMS) [2], or the conventional elastic polymer material used for soft lenses [3]. PDMS was pinpointed as a good candidate because it is nonreactive, does not usually cause any eye irritation or secondary reactions, and has been used in the fabrication of very small circuit patterns for many years. It is also transparent and durable. The conventional elastic polymer in use for smart contact lens development is known to be flexible, permeable to oxygen, and transparent [3]. While this second material gives added comfort and thinness due to its flexibility, it comes with trade-offs. Such a flexible material is also prone to distortion. To mitigate the risk of distortion of the contact lens, reinforcement bits are mixed into the polymer medium to give the contact more structure without compromising its transparency [3]. The flexible base prevents tears and absorbs any stress from stretching the contact, and the reinforcement bits prolong the life of the contact and augment its functionality [3].
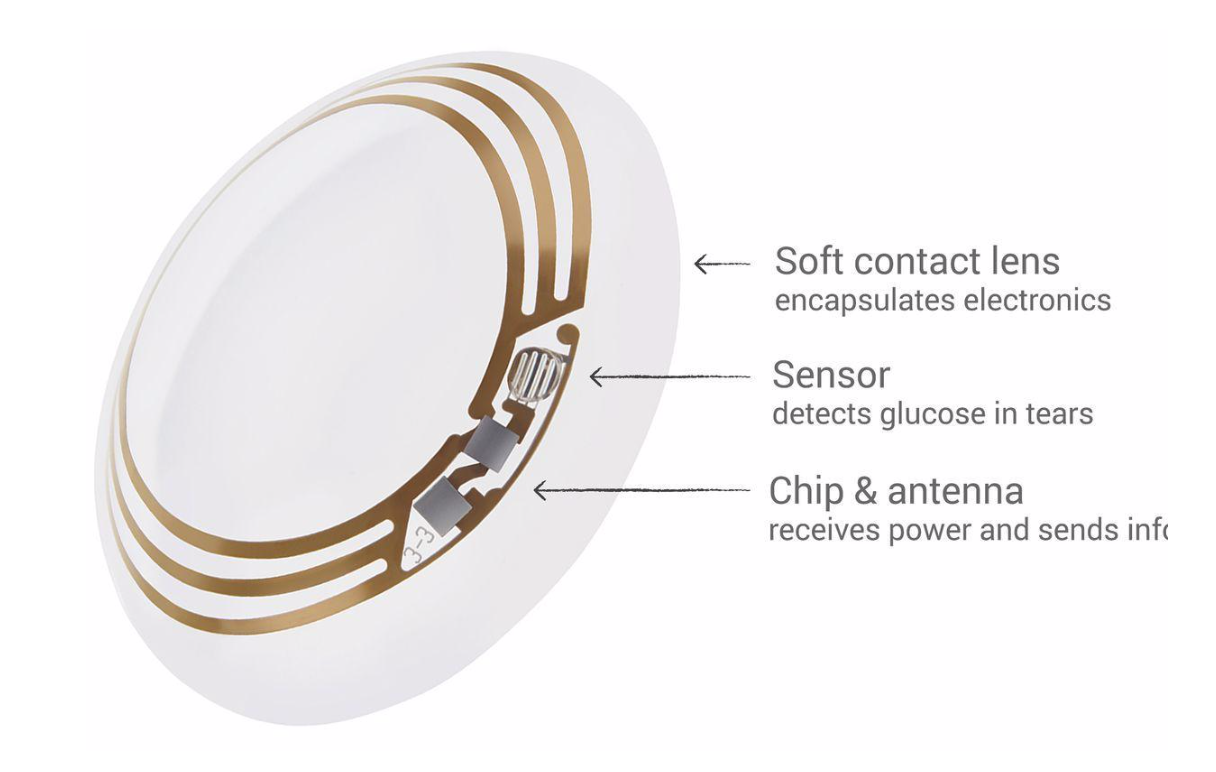
Beyond its main foundation, the smart contact requires the components that make it “smart.” These include the conductive (circuit) layer, any sensors or chips, and ligands—molecules attached to a metal carrier for the purpose of attracting other molecules—that bind any specific molecules for which the contact may be searching. Figure 1 depicts a typical smart contact layout.
Figure 1. Typical smart contact lens layout. [4].
The conductive layer is standardized among smart contacts and is usually made of a thin coat of gold or silver. The required sensors depend on the function of the smart contact — for example, a contact designed to measure pressure and requires pressure gauges. In some cases, the contact needs to determine the composition of the wearer’s tears or test for a specific molecule in those tears. In that case, the contact can be seeded with ligands that will bind to the target molecule (or with small molecules of metal that will catalyze the target reaction) [5].
Finally, all smart contacts are wireless, which means they need a way to communicate the information they collect about molecules, eye pressure, or any other relevant data. The RF antenna serves this purpose and must also be built into the contacts. If any information is going to be stored in the contact before transmission to the outside information receiver, the contact needs a memory chip as well. All of these different electronic components (the metal film, the sensors, the memory chip, and the antenna) need to be efficiently connected, and the frequency that transmits the data from the lens to the final data storage location must be safe for the human eye [2].
Fabrication Technique
Smart contacts have employed the microelectromechanical system (MEMS) fabrication techniques [2]. MEMS are miniscule electronic devices, usually comparable in size to a single red blood cell. Because MEMS (and the circuitry for these contacts) are so small, it is important that not even one dust particle gets into the system. They are made in clean rooms where all of the workers in the lab have to wear marshmallow suits that cover their clothing, hair, and face. The lab has engineered its direction of air flow so that any particles floating through the air are funneled directly to the floor and removed from the room rather than floating into the devices. All of the smart contact manufacturing has to be completed in clean rooms like this.
The PDMS of the contact lens is coated with a thin sheet of metal that will form the electronic connection in the contact’s circuit. Then the lens undergoes a series of complex mechanisms that together are called “photolithography”, as explained in Figure 2, and the exact pattern for the desired circuit is left behind on the PDMS [2].
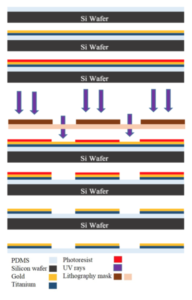
Figure 2. The Steps to Photolithography – PDMS contact lenses are coated with metal and a light sensitive chemical called photoresist. A mask of the desired circuitry is laid on top of these layers and ultraviolent lights cures the photoresist. The layers are washed away, and left behind in metal is the circuit pattern for the contact lens [2].
However, circuitry does not only refer to the design of the smart contacts. If the contact is supposed to be probing for the presence of molecules in the tears, then the contact can be seeded with indicator molecules that will react with those molecules being searched for. The indicator can be a color change, or can tie into circuitry so that the quantity of the target molecule will be transmitted through the RF antenna [2]. Other possible applications utilizing MEMS fabrication technology with indicators are drug-eluting smart contacts, or contacts that contain a reservoir of medication to be delivered when necessary. If the contact is designed to deliver a drug, an activating or catalyzing molecule can cause the drug to be administered [5]. Capillary action, or the tendency for small “pipes” to easily hold and release a liquid, can be used to store the drug, and an indicator that changes color lets wearers or doctors know the drug has been delivered.
These fabrication techniques are common to all smart contacts, but there is still new research attempting to optimize contact performance and minimize damage to the eyes. The leading research in the new wave of smart contacts suggests using graphene as part of the contact base [5]. Graphene is biocompatible, transparent, and has good mechanical properties that make it a viable option for a contact lens material. New research suggests that it can dissipate electromagnetic radiation from the sun and its heat so that the contact lens receives the brunt of the damage, rather than the patient’s eye [6] (Figure 3). While this is not yet a health concern, it could be an avenue for preventative ocular medicine in the future. Researchers also claim that it prevents dehydration of the eye, which is important given that most contact wearers suffer from dry eyes due to contact use [6]. However, research has not yet indicated whether or not a new generation of graphene-based contacts will be oxygen permeable. While all the presented information seems positive, there have not yet been pilot smart contacts made of graphene tested in a clinical setting.
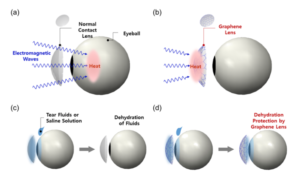
Figure 3. Benefits of Using Graphene for Smart Contact Fabrication [6].
Applications
As suggested above, many potential applications for smart contacts exist. These include the disease diagnosis and treatment for which they are being tested, further biomedical applications for diseases that have not been tested, and everyday use in preventative healthcare or recreation.
The first of these categories, disease treatment and diagnosis, is the one for which we have the most data. If the contacts are fitted with pressure sensors, then they can test for glaucoma—a disease in which there is increased pressure in a person’s eye. Extra strain on the surface of the eye, and therefore the contact, is easy to monitor using a lens [7]. The contacts can also be fitted with specific molecule sensors — for instance, including glucose sensors can monitor blood sugar levels in diabetic patients [8]. Lastly, the contact can hold a small reservoir of medicine and release it in response to a specific stimulus built into the design [9]. All of these uses for smart contacts make patient monitoring easier and constant monitoring [2] possible. This is especially important for elderly patients. Elderly patients often suffer more from ailments like glaucoma or diabetes, but have more difficulty traveling to the doctor’s office. If there is a way for them to receive the medicine they need without having to go into the doctor’s office (or a way for their doctor to monitor their glucose levels or eye pressure), it affords them a better quality of life without compromising their healthcare.
A more common application for smart contacts is to combat eye fatigue. Ophthalmologist Dr. Michele Andrews claims that phone and computer screens cause “digital eye fatigue”, tiredness, and dry eyes [10]. A smart contact company called Bioinfinity Energys has designed a contact meant to help the average person switch their focus between digital screens and the real world [10]. If both of these claims are true, then there is a much larger market for the smart contact lens within the medical community than pioneer researchers originally believed.
Finally, as with all new inventions, there is a niche for smart contacts simply as a novel technology. Most medical devices are the brain-child of an immediate stress (in this case quality and speed of care) and then later expand to mainstream use. In their mainstream phase, these contacts could be used as a health monitoring device much like a Fitbit, and will probably become the first step towards computer integration with the human body. Soon, we may all be cyborgs capable of saving the world—Avengers here we come!
References
[1] C. Hastings, “Smart Contact Lenses are Here: Interview with Prof. Herbert De Smet of Imec
|,” Medgadget, 13-Dec-2018. [Online].
[2] K. Burgess, A. Kraft, and G. R. Stephenson, “Biomedical, Advanced Materials, Organic
Chemistry,” Feb-2014.
[3] S.-Y. K. Joohee Kim, W. H. Cheong, Y.-T. K. Kyungmin Na, J. H. Heo, C. Y. Lee, J. H.
Lee, and J.-U. P. Franklin Bien, “Soft, smart contact lenses with integrations of wireless
circuits, glucose sensors, and displays,” Science Advances, 01-Jan-2018. [Online].
[4] J. Temple, “Inside Google X’s Smart Contact Lens,” Recode, 16-Jan-2014. [Online]
[5] S. Tinku, C. Collini, L. Lorenzelli, and R. S. Dahiya, “Smart contact lens using passive
structures,” IEEE Explore Digital Library, 02-Nov-2014. [Online].
[6] “Smart Contact Lenses with Graphene Coating for Electromagnetic Interference Shielding
and Dehydration Protection,” ACS Publications. [Online].
[7] “University of California – Davis; Smart contact lense,” VerticalNews, 31-Aug-2008.
[8] “From smart contact lenses to supercooled silicon,” Nature Materials, Feb-2004.
[9] Editors, “Drug Releasing Contact Lens Changes Color to Show When Its Working
|,” Medgadget, 12-Oct-2018. [Online].
[10] M. Batista, “CooperVision’s Contacts Combat Eye Fatigue from Digital Screen Usage
(Interview) |,” Medgadget, 29-Oct-2018. [Online].